Causes of itching and peeling of interdigital folds
- Trichophyton (T. rubrum, T. interdigitale, T. violaceum).
- Epidermophyton (E. floccosum).
- Mold.
Predisposing factors
- Excessive sweating (hyperhidrosis).
- Incorrect shoe selection (uncomfortable, made of synthetic material).
- Anatomical features of the foot (flat feet, tight folds).
- Bruising and diaper rash are present.
- Damage (mechanical damage, chemical damage).
Podomycoses, skin lesions between the toes, are caused by fungi and occur in the context of local or systemic disease.
What does mycosis look like?
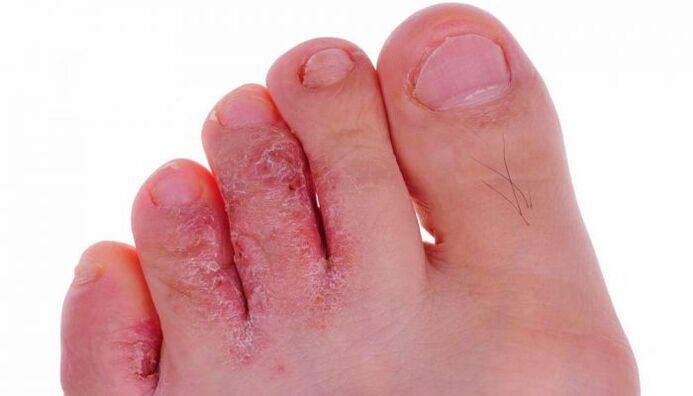
- Squamous.
- rub against each other.
- Sweating disorders.
Lesions of the interdigital space often occur simultaneously with other forms of podiatry, suggesting the unity of the pathological process.
diagnosis
How to Treat Sores?

- Wear comfortable, breathable shoes.
- Wear cotton socks.
- Dry your feet after showering and bathing.
- Use personal slippers in public places.
Effective creams and ointments
If your skin becomes wet and cracks

If fungal lesions develop on the skin of the feet, external treatment with antifungals, antiseptics, and antibiotics is essential.
pill
What can be done with folk remedies?
- Apple cider vinegar (1 cup per 3 liters of hot water) and club soda (5 tablespoons).
- Potassium permanganate (1 g/2 liters).
- Calendula soup (250g/2L).
















